You are navigating the complex landscape of your brain, and sometimes, that landscape experiences unexpected geological shifts. One such shift can occur in the temporal lobes, the brain’s primary processing centers for memory, emotion, and sensory information. When these areas become abnormally electrically active, you might be experiencing temporal lobe epilepsy (TLE). Understanding the patterns that emerge from these electrical disturbances is crucial for diagnosis, treatment, and ultimately, for regaining control over your neurological well-being. This article aims to demystify these brain patterns, offering you a clearer picture of what’s happening within your temporal lobes.
Your temporal lobes, situated beneath your temples, are like busy transit hubs for your brain. They are responsible for a vast array of crucial functions, acting as the brain’s interpreters of sensory input and the architects of your memories.
The Architecture of the Temporal Lobe
Structurally, the temporal lobe is a sophisticated network of interconnected regions. Key players include:
The Hippocampus: The Memory Keeper
At the heart of the temporal lobe lies the hippocampus, a seahorse-shaped structure that acts as a central processor for forming new explicit memories, those you can consciously recall. Think of it as the brain’s librarian, meticulously cataloging every new piece of information. Dysfunctions here can profoundly impact your ability to learn and remember.
The Amygdala: The Emotion Regulator
Adjacent to the hippocampus is the amygdala, a pair of almond-shaped clusters of nuclei. This is your brain’s emotional alarm system, responsible for processing fear, pleasure, and other strong emotions. It’s the conductor of your emotional orchestra, influencing your mood and reactions. When the amygdala becomes overactive in TLE, you might experience intense fear, anxiety, or even a sense of dread during seizures.
The Auditory Cortex: The Sound Decoder
Within the temporal lobe, the auditory cortex is dedicated to processing sound. It’s your brain’s ear, deciphering the nuances of spoken language, music, and environmental noises. Abnormal electrical activity here can manifest as auditory hallucinations, such as hearing voices or sounds that aren’t present.
The Visual Cortex: The Visual Interpreter (Partial Involvement)
While the primary visual cortex resides in the occipital lobe, the temporal lobe also plays a role in visual processing, particularly in recognizing objects and faces. Lesions or electrical disturbances impacting these pathways can lead to visual disturbances during a seizure.
The Symphony of Normal Brain Activity
In a healthy brain, the temporal lobes hum with a synchronized electrical symphony. Neurons communicate through precisely timed electrical impulses, creating intricate patterns that support your daily functions. This electrical activity can be measured and visualized through electroencephalography (EEG), revealing distinct brainwave frequencies.
Alpha Waves: The Calm State
When you are relaxed but awake, your EEG will show prominent alpha waves, characterized by their moderate frequency and amplitude. This is your brain’s state of quiet observation.
Beta Waves: The Active Mind
As your brain becomes more engaged in tasks, problem-solving, or focused attention, beta waves become more dominant. These are faster and smaller than alpha waves, reflecting active cognitive processing.
Theta Waves: The Drowsy or Deeply Meditative State
Theta waves emerge as you transition into sleep or enter a state of deep meditation. They are slower and larger than alpha waves, indicating a more relaxed or introspective brain state.
Delta Waves: The Deep Sleep
During the deepest stages of non-REM sleep, your brain produces slow, high-amplitude delta waves. This is the period of profound rest and physical restoration.
Recent studies have shed light on the intricate brain patterns associated with temporal lobe epilepsy, revealing how abnormal electrical activity can influence cognitive functions and emotional regulation. For a deeper understanding of these phenomena, you can explore a related article that discusses the implications of these findings on treatment approaches and patient outcomes. To read more, visit this article.
Unraveling the Electrical Storms of TLE
Temporal lobe epilepsy is characterized by recurrent, unprovoked seizures that originate in these lobes. The hallmark of TLE is the presence of abnormal, excessive, and synchronous neuronal discharges that disrupt the brain’s normal electrical chatter. Understanding these patterns is like deciphering a secret code, revealing the locus and nature of the seizure activity.
Interictal Discharges: The Whispers Before the Roar
Even between seizures, your temporal lobes can exhibit subtle electrical abnormalities known as interictal epileptiform discharges (IEDs). These are like faint murmurs in the otherwise quiet theater of your brain, hinting at underlying electrical instability.
Spikes and Sharp Waves: The Anomalous Signals
IEDs typically manifest as pointed, brief deflections on an EEG, known as spikes or sharp waves. These are deviations from the normal smooth flow of brain activity, representing a small population of neurons firing erratically.
Polyspikes: The Echo of Aberrant Firing
Sometimes, you might observe a series of closely spaced spikes, termed polyspikes. This pattern suggests a brief burst of synchronized, abnormal neuronal firing.
Slow Waves: Prolonged Disturbance
In some instances, interictal abnormalities can also present as slow waves, indicating a more sustained period of disrupted electrical activity in a localized area.
Identifying these interictal patterns is crucial. They can help pinpoint the affected temporal lobe (left or right) and sometimes even a more specific region within the lobe, guiding your medical team in their diagnostic efforts.
Ictal Discharges: The Seizure’s Electrical Fingerprint
When a seizure actually occurs, the electrical activity in your temporal lobe undergoes a dramatic transformation. This is the “ictal phase,” the storm itself, and its EEG signature is unmistakable.
Focal Onset Motor Seizures: The Physical Manifestations
If the seizure begins with a focal onset motor seizure originating in the temporal lobe, you might experience involuntary muscle movements, such as twitching or jerking of a limb or facial muscles. The EEG will typically show rhythmic, repetitive spike and wave activity in the temporal region corresponding to the affected motor pathway.
Focal Onset Non-Motor Seizures (With or Without Impaired Awareness): The Introspective and Sensory Alterations
These seizures can be more subtle and are often characterized by alterations in sensation, emotion, cognition, or autonomic functions. The EEG patterns here are diverse and can include:
Aura: The Precursor to the Event
Many individuals with TLE experience an aura, a type of focal awareness seizure, preceding a more generalized seizure. This aura itself is an ictal event, characterized by distinct electrical patterns. For instance, if the seizure originates in the hippocampus, you might experience a sensation of rising nausea, déjà vu, or a peculiar smell or taste. The EEG can capture rhythmic or evolving rhythmic sharp waves, slow waves, or spiking activity localized to the mesial temporal lobe.
Dissociative Automatisms: The Unconscious Performances
During a seizure with impaired awareness, you might engage in automatisms, which are complex, repetitive, involuntary behaviors like lip-smacking, chewing, fumbling with clothing, or even walking. The EEG during these episodes often shows focal rhythmic slowing, sometimes interspersed with spikes, originating in the temporal lobe. Think of these as involuntary performances dictated by the electrical storm, with you as an unwitting actor.
Sensory Hallucinations: The Brain’s Phantom Inputs
As mentioned, the auditory cortex can be involved, leading to hallucinations of sounds or voices. The EEG might reveal rhythmic discharges in the temporal lobe, often the superior temporal gyrus, correlating with these auditory experiences. Similarly, visual disturbances can manifest with patterns in the visual processing areas of the temporal lobe.
Emotional Aberrations: The Surge of Uncontrolled Feelings
The amygdala’s involvement can lead to sudden and intense feelings of fear, anxiety, panic, or even inexplicable joy. The EEG can show abnormal activity in the basolateral amygdala region, contributing to these profound emotional shifts. Your emotional barometer is being wildly and uncontrollably swung by the electrical surges.
Secondary Generalization: The Electrotonic Contagion
In some cases, a focal seizure originating in the temporal lobe can spread to involve both hemispheres of the brain, leading to a generalized tonic-clonic seizure. This is like a spark igniting a wildfire; the abnormal electrical activity escapes its temporal lobe confines and engulfs the entire brain. The EEG will initially show focal activity in the temporal lobe, which then evolves into the characteristic generalized spike-and-wave pattern of a tonic-clonic seizure.
Postictal State: The Lingering After-Effects
Following a seizure, your brain enters a “postictal” period, characterized by temporary neurological deficits and altered mental status. This is akin to the calm after the storm, but with residual effects.
Confusion and Drowsiness: The Brain’s Recovery Phase
You might experience confusion, disorientation, and significant drowsiness as your neurons recover from the intense electrical activity. The EEG during this phase often shows generalized slowing, reflecting the brain’s effort to return to normal function.
Memory Gaps: The Amensia Post-Event
Difficulty recalling events leading up to or immediately following the seizure is common, especially if the hippocampus was involved. This is the librarian needing time to reshelve all the books after a chaotic rush.
Diagnostic Tools: Capturing the Brain’s Evolving Patterns
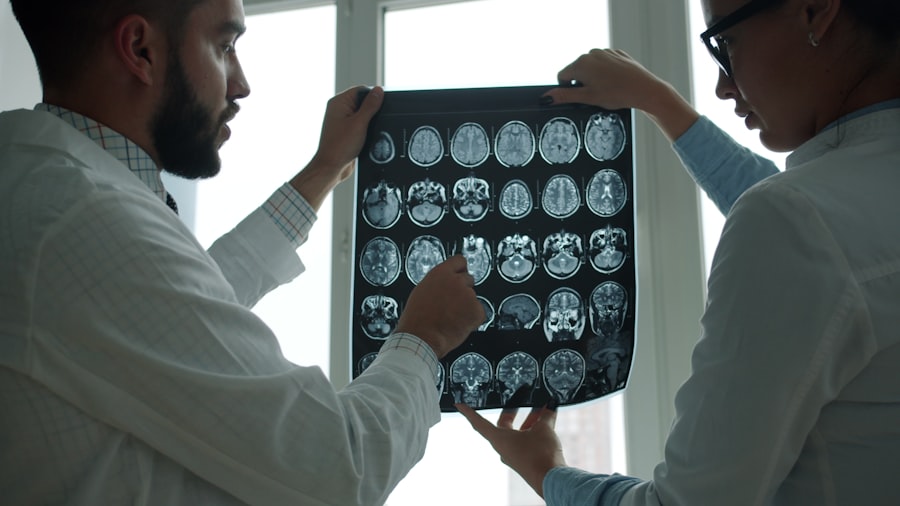
To understand the brain patterns in TLE, various diagnostic tools are employed, with electroencephalography (EEG) taking center stage.
Electroencephalography (EEG): The Brain’s Electrical Scroll
EEG is the primary method for detecting and analyzing abnormal electrical activity in the brain. Sensors (electrodes) are placed on your scalp to record the collective electrical impulses of millions of neurons.
Routine EEG: A Snapshot of Brain Activity
A routine EEG, typically lasting 20-40 minutes, provides a snapshot of your brain’s electrical activity. While it can capture interictal discharges, it may not always record a seizure if one is not occurring during the recording period.
Video EEG Monitoring: The Continuous Surveillance
For a more comprehensive evaluation, particularly to correlate brain activity with your symptoms, video EEG monitoring is often recommended. This involves continuous EEG recording, sometimes for several days, coupled with video documentation of your behavior. This allows clinicians to precisely link specific EEG patterns to the events you experience. It’s like having a silent, tireless observer documenting the unfolding drama within your brain.
Long-Term Monitoring: The Extended Watch
In some challenging cases, long-term monitoring in a specialized epilepsy unit may be necessary to capture infrequent seizures and gain a deeper understanding of your seizure patterns.
Magnetic Resonance Imaging (MRI): Mapping the Brain’s Landscape
While EEG reveals the electrical activity, MRI provides detailed structural images of your brain. This is crucial for identifying underlying causes of TLE, such as:
Hippocampal Sclerosis: The Scarred Memory Center
A common finding in TLE is hippocampal sclerosis, a form of scarring and neuronal loss in the hippocampus. MRI can often detect this, providing a physical explanation for the seizure origin.
Lesions and Malformations: The Structural Anomalies
MRI can also identify other structural abnormalities like tumors, vascular malformations, or congenital malformations that might be contributing to the epilepsy.
Understanding the Temporal Location: Left vs. Right TLE
The side of your temporal lobe from which seizures originate can influence the types of symptoms you experience. This distinction is crucial for surgical planning if operative intervention is considered.
Left Temporal Lobe Epilepsy: The Linguistic Labyrinth
The left temporal lobe is dominant for language in most individuals. Seizures originating here can often manifest with:
Aphasia and Speech Difficulties: The Unraveling of Words
You might experience difficulties speaking, understanding language, or finding the right words during a seizure. This can range from subtle word-finding problems to complete aphasia.
Memory Disturbances Affecting Verbal Recall: The Fraying of Verbal Memories
Your ability to recall verbal information might be more significantly affected if the left hippocampus is involved.
Right Temporal Lobe Epilepsy: The Spatial and Emotional Canvas
The right temporal lobe is more involved with spatial processing, visuospatial awareness, and emotional processing. Seizures here can lead to:
Visuospatial Impairments: The Distortion of Space
You might experience difficulties with spatial navigation, recognizing faces, or perceiving visual information accurately.
Emotional and Affective Changes: The Unpredictable Emotional Rollercoaster
Intense emotional outbursts, sudden fear, or other mood alterations can be more pronounced with right-sided TLE.
Recent studies have shed light on the intricate brain patterns associated with temporal lobe epilepsy, revealing how these patterns can influence both seizure activity and cognitive functions. For a deeper understanding of this topic, you can explore a related article that discusses the implications of these findings on treatment approaches and patient outcomes. This insightful piece can be found here, providing valuable information for those interested in the neurological aspects of epilepsy.
Therapeutic Strategies: Harnessing Knowledge to Control Seizures
| Metric | Description | Typical Findings in Temporal Lobe Epilepsy (TLE) | Measurement Method |
|---|---|---|---|
| Interictal Epileptiform Discharges (IEDs) | Abnormal spikes or sharp waves between seizures | Increased frequency localized to temporal lobe regions | EEG (Electroencephalography) |
| Hippocampal Atrophy | Volume loss in the hippocampus | Significant reduction in hippocampal volume on affected side | MRI (Magnetic Resonance Imaging) |
| Functional Connectivity | Synchronization between brain regions | Altered connectivity between temporal lobe and limbic structures | fMRI (Functional MRI), MEG (Magnetoencephalography) |
| Seizure Onset Zone | Region where seizures originate | Localized to mesial or lateral temporal structures | Intracranial EEG, PET (Positron Emission Tomography) |
| Gamma Oscillations | High-frequency brain waves (30-100 Hz) | Increased gamma activity during seizures in temporal lobe | EEG, Intracranial EEG |
| Neuronal Loss | Reduction in neuron density | Marked neuronal loss in CA1 and CA3 hippocampal subfields | Histopathology (post-surgical tissue analysis) |
Understanding the specific brain patterns associated with your TLE is the bedrock upon which effective treatment strategies are built. The goal is to either suppress the abnormal electrical activity or, in select cases, surgically remove the epileptogenic zone.
Pharmacological Treatments: The Neurochemical Regulators
Anti-epileptic drugs (AEDs) are the first line of treatment for most individuals with TLE. These medications work by altering the balance of neurotransmitters in your brain to reduce neuronal excitability.
Targeting Excitatory and Inhibitory Balance: The Fine-Tuning of Neuronal Communication
AEDs aim to either increase the brain’s inhibitory mechanisms or decrease its excitatory ones, essentially acting as brakes and dampeners on the runaway electrical activity. Different drugs have different mechanisms of action, and finding the right one for you involves careful titration and monitoring.
Surgical Interventions: The Precision Removal of the Source
For individuals with drug-resistant TLE, epilepsy surgery can be a highly effective option. This involves precisely identifying and removing the area of the brain that is generating the seizures.
Resective Surgery: Upgrading the Brain’s Hardware
This is the most common type of epilepsy surgery. Based on extensive pre-surgical evaluation, including EEG and MRI findings, the epileptogenic zone is surgically removed. It’s like a skilled mechanic identifying a faulty component in your engine and replacing it.
Laser Interstitial Thermal Therapy (LITT): The Minimally Invasive Solution
A more minimally invasive surgical technique, LITT uses a laser to heat and destroy small areas of abnormal brain tissue causing seizures. This offers a less invasive approach with potentially faster recovery.
Neuromodulation Therapies: The Advanced Brain Tuning
When surgery is not feasible, or as an adjunct to other treatments, neuromodulation techniques can be employed.
Vagus Nerve Stimulation (VNS): The External Pacemaker for Neuronal Activity
VNS involves implanting a device that sends electrical impulses to the vagus nerve, which in turn influences brain activity. This can help reduce seizure frequency and severity.
Deep Brain Stimulation (DBS): The Targeted Electrical Intervention
DBS involves implanting electrodes in specific brain regions to deliver targeted electrical stimulation, helping to regulate abnormal brain activity.
By understanding the intricate electrical patterns that characterize temporal lobe epilepsy, you gain a powerful advantage in your journey toward managing this condition. This knowledge empowers you to work collaboratively with your medical team, explore treatment options, and ultimately, to reclaim the intricate symphony of your brain’s normal rhythms.
FAQs
What is temporal lobe epilepsy?
Temporal lobe epilepsy (TLE) is a neurological disorder characterized by recurrent seizures originating in the temporal lobes of the brain, which are involved in processing emotions, memory, and sensory input.
How do brain patterns differ in individuals with temporal lobe epilepsy?
Individuals with temporal lobe epilepsy often exhibit abnormal electrical activity in the temporal lobes, including interictal epileptiform discharges and altered connectivity patterns, which can be detected using EEG or neuroimaging techniques.
What role do brain patterns play in diagnosing temporal lobe epilepsy?
Brain patterns, such as specific seizure-related electrical discharges and changes in brain wave rhythms, are critical for diagnosing TLE. These patterns help clinicians localize the seizure focus and differentiate TLE from other types of epilepsy.
Can brain pattern analysis help in predicting seizures in temporal lobe epilepsy?
Yes, analyzing brain patterns can sometimes help predict seizures by identifying preictal (before seizure) changes in brain activity, although this is an area of ongoing research and not yet fully reliable for all patients.
How does understanding brain patterns impact the treatment of temporal lobe epilepsy?
Understanding brain patterns in TLE can guide treatment decisions, such as selecting appropriate medications, planning surgical interventions, or using neurostimulation therapies, by targeting the specific areas and networks involved in seizure generation.